| 图片: | |
|---|---|
| 名称: | |
| 描述: | |
- B494UPSC1例
| 姓 名: | 患者 | 性别: | 女 | 年龄: | 67 |
| 标本名称: | 宫腔内肿瘤 | ||||
| 简要病史: | 绝经20年,阴道出血 | ||||
| 肉眼检查: | 宫腔内小乳头状肿块,切面未见明显肌层浸润 | ||||
1 2 3 4
5 6 7 8
9 10 11 12
13 14 15 16
17 18 19 20
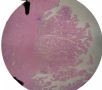
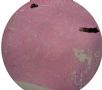
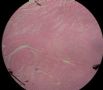
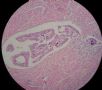
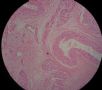
图1为全貌。图2-7显示浅肌层。图7-10显示深肌层。图11-14显示近浆膜面肌层。图15为图3的局部放大。图16为图5和图6的局部放大。图17为图7的局部放大。图18为图12的局部放大。图19为图11的局部放大。
-
本帖最后由 于 2006-12-15 12:33:00 编辑

华夏病理/粉蓝医疗
为基层医院病理科提供全面解决方案,
努力让人人享有便捷准确可靠的病理诊断服务。
相关帖子
- • 来一例简单罕见的(有诊断)
- • 是肉瘤吗?
- • 子宫内膜,复杂性增生?癌?(有大体结果了)
- • 子宫肿物(透明细胞平滑肌瘤?)
- • 子宫肌壁间肿物
- • 子宫腔内占位。
- • 子宫肿瘤
- • 子宫肌层浸润性癌
- • 8 个子宫上皮肿瘤病例-扫描图片
- • 子宫平滑肌肿瘤?间质肉瘤?
-
本帖最后由 于 2007-05-09 22:34:00 编辑
Uterine Papillary Serous Carcinoma
E. Cagnur Ulukus, M.D., John R. Davis, M.D., and Setsuko K. Chambers, M.D.
很抱歉由于版权问题,不能引用全文。以下各图均引自此文,谨向郑文新老师(Wenxin Zheng, M.D.)致谢!感谢wangzhen_01提供资料!
zhjjwf 译:
子宫内膜腺体不典型增生先于子宫浆液性乳头状癌的出现
摘要:子宫内膜腺体不典型增生(EmGD)是一个新的概念体系,它通常与浆液性子宫内膜上皮内癌和子宫内膜浆液性乳头状癌(UPSC)有特定的联系.有人建议将子宫内膜腺体不典型增生看作UPSC的一种真正的癌前病变,根据我们最近的研究显示两者在形态学和分子水平有关联。本研究应用回顾性研究方式,通过观察它们的临床病理特征,以检测是否EmGD出现在UPSC发展之前,并界定从EmGD的出现到充分发展为UPSC的时期。250例UPSC 和258例良性病例被用于本次研究。为了鉴定是否EmGD 出现在UPSC 之前,我们重新观察了所有可得到的子宫切除前3个月或更早的子宫内膜活检标本。这包括来自UPSC的27例活检标本和29例良性对照组的标本。那些在子宫内膜形态学上异常,与原来活检时的诊断一致且符合EmGD的病例,将被记录下来。在所有子宫切除前的内膜活检标本中,我们在形态学上确诊为EmGD的共10例;包括27例UPSC组中的9例(33%),29例良性对照组中的1例。除1例来自UPSC组未进行检测和1例来自良性对照组的得分为0分外,10例形态学上诊断为EmGD的病例均显示p53染色的高得分(5分)。
所有EmGD病例均表现为高MIB-1指数,但形态上表现为良性的病例则为低的MIB-1指数。本研究的主要目的是回顾性地研究这些确诊为EmGD的病例。从确诊为EmGD到出现子宫内膜上皮内浆液性癌或完全发展为UPSC的时间为16到98个月,平均为33个月。我们得出结论,EmGD的出现早于UPSC的发生。这一发现支持了我们最近提出的UPSC发展模型建议,这一模型认为EmGD很可能是UPSC的癌前病变。更深入的研究需要集中探讨其分子及细胞学机制、可逆性和UPSC发展的危害和EmGD的临床处理。

华夏病理/粉蓝医疗
为基层医院病理科提供全面解决方案,
努力让人人享有便捷准确可靠的病理诊断服务。
-
zhongshihua 离线
- 帖子:1608
- 粉蓝豆:0
- 经验:1651
- 注册时间:2006-09-11
- 加关注 | 发消息
-
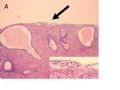
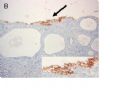
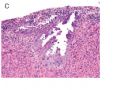
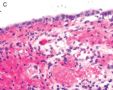
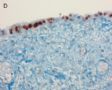
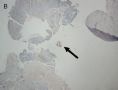
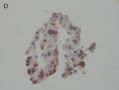
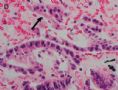
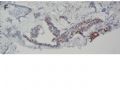
FIG. 1. Endometrial biopsy 16 months before hysterectomy in case 1. Focal areas of EmGD lining on the surface of an otherwise unremarkable endometrial polyp were seen (A, arrow). Mild-to-moderate degree of atypia of the EmGD cells was better appreciated in a high-power view (insert in the upper right corner of A). Immunohistochemistry of p53 staining (B and a magnified picture in the insert) highlighted the EmGD cells with a score of 7 (percentage 2, intensity 3, and heterogeneity 2). The resting endometrial glands within the endometrial polyp in Figure

华夏病理/粉蓝医疗
为基层医院病理科提供全面解决方案,
努力让人人享有便捷准确可靠的病理诊断服务。
FIG. 2. Endometrial glandular dysplasia glands in an endometrial polyp of case 2. The endometrial biopsy was performed 17 months before the hysterectomy. Figure

华夏病理/粉蓝医疗
为基层医院病理科提供全面解决方案,
努力让人人享有便捷准确可靠的病理诊断服务。
-
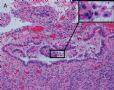
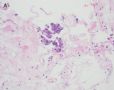
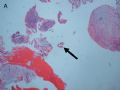
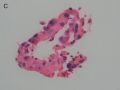
FIG. 3. Endometrial glandular dysplasia glands on the surface of atrophic endometrium in case 3. The endometrial biopsy sample showed several strips of atrophic endometrium. One piece of the atrophic endometrium contained 2 foci of EmGD with 1 on the surface (A with arrow). One piece of them showed 2 foci of EmGD with 1 on the surface (A with arrow) and the other showed 2 small papillary fronds (in the center of Fig.

华夏病理/粉蓝医疗
为基层医院病理科提供全面解决方案,
努力让人人享有便捷准确可靠的病理诊断服务。
-
FIG. 4. The endometrial biopsy of case 4 performed 21 months before the hysterectomy. Figure

华夏病理/粉蓝医疗
为基层医院病理科提供全面解决方案,
努力让人人享有便捷准确可靠的病理诊断服务。
-
本帖最后由 于 2007-05-01 23:02:00 编辑
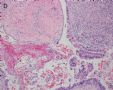
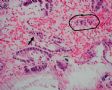
FIG. 5. Case 5 with EmGD lesions in an endometrial biopsy 16 months before the hysterectomy. The specimen showed several fragments of endometrial polyp (A). There was 1 small fragment of the endometrium (arrow in A) showing atypical cells with a relatively large amount of eosinophilic cytoplasm (magnified view in Fig.

华夏病理/粉蓝医疗
为基层医院病理科提供全面解决方案,
努力让人人享有便捷准确可靠的病理诊断服务。
FIG. 6. Endometrial glandular dysplasia lesion in an endometrial biopsy specimen 26 months before the hysterectomy from case 6. The lesion was indicated by an arrow in Figure

华夏病理/粉蓝医疗
为基层医院病理科提供全面解决方案,
努力让人人享有便捷准确可靠的病理诊断服务。






















 提议斑竹将此贴设为精华贴!
提议斑竹将此贴设为精华贴!